Key Takeaways
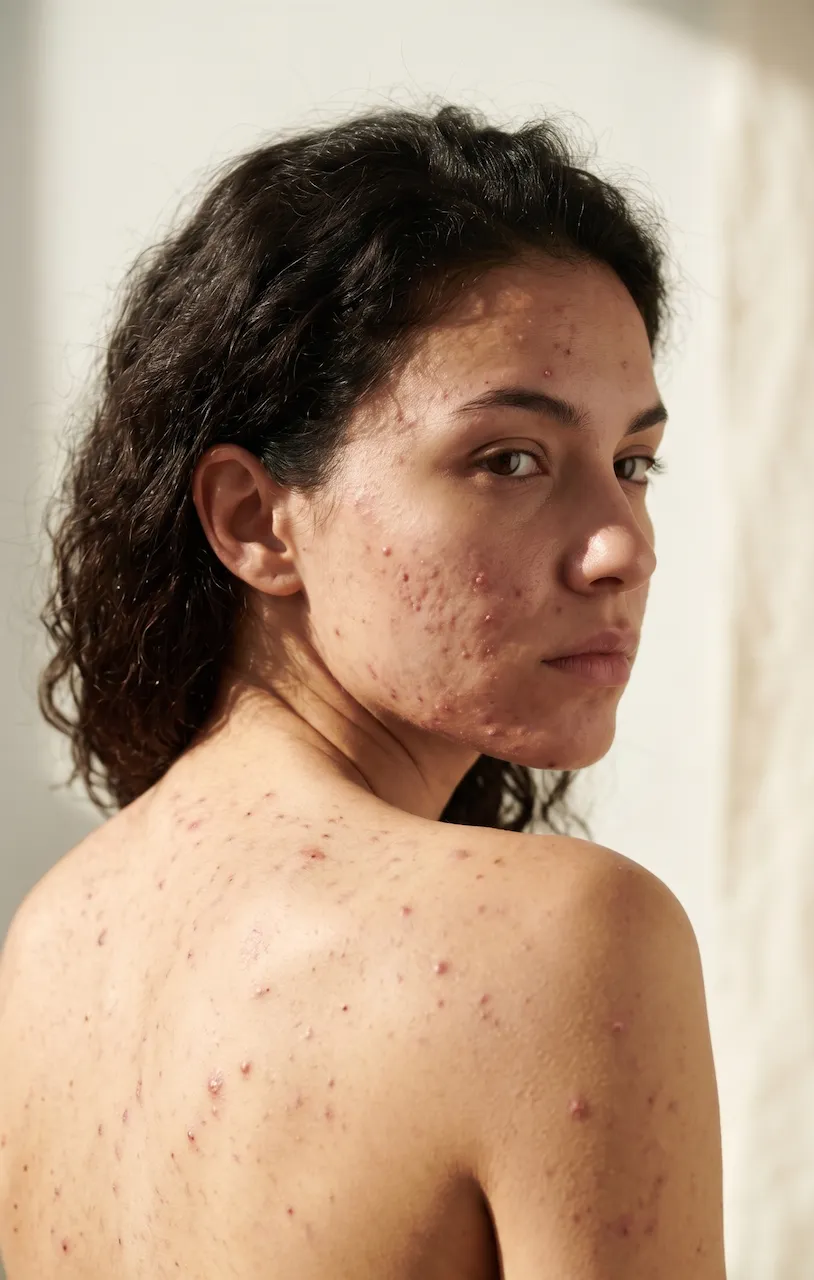
If you are a woman dealing with breakouts across your back and shoulders, you are not alone — and you are not imagining that it seems to flare at the worst possible times. Back acne in females is incredibly common, and the frustration of not understanding why it keeps coming back can feel just as overwhelming as the breakouts themselves.
While the basic mechanism behind all acne is the same — clogged pores, excess oil, bacteria, inflammation — what causes back acne in females often has a distinctly hormonal component. Fluctuating estrogen and progesterone levels during the menstrual cycle, androgen imbalances linked to conditions like PCOS, and hormonal shifts during pregnancy or perimenopause all play roles that are unique to the female experience. On top of that, lifestyle factors like clothing choices, workout habits, and skincare products can make things worse.
Understanding the specific causes behind your back acne is the first step toward treating it effectively. Below, we will walk through the hormonal, lifestyle, and genetic factors that drive back acne in females, how they differ from the causes in males, and what treatment options actually work.
Quick Answer: What Causes Back Acne in Females?
The short version: Back acne in females is most commonly caused by hormonal fluctuations — particularly shifts in androgens, estrogen, and progesterone — combined with the back's naturally high concentration of oil glands.
Key hormonal triggers include:
- Menstrual cycle: Progesterone rises before your period, increasing oil production and premenstrual flares
- PCOS: Elevated androgens drive excess sebum and persistent breakouts
- Stress hormones: Cortisol stimulates oil glands and worsens inflammation
- Pregnancy and perimenopause: Major hormonal shifts can trigger new or worsening back acne
Common lifestyle triggers: Tight clothing, post-workout sweat, hair products, and pore-clogging body care products
Hormonal Causes of Back Acne in Females
Hormones are the single biggest differentiator when it comes to what causes back acne in females versus other populations. While all acne has a hormonal component — androgens stimulate oil production in everyone — females experience a unique pattern of hormonal fluctuations throughout the menstrual cycle, during pregnancy, and during the transition to menopause that directly influence breakout patterns.
The Menstrual Cycle and Premenstrual Flares
If your back acne seems to get worse in the week or two before your period, you are not imagining it. Research published in the Archives of Dermatological Research has confirmed that premenstrual acne flares are a well-documented phenomenon, affecting an estimated 44-83% of women with acne.
Here is what happens hormonally: During the luteal phase of your menstrual cycle (roughly the two weeks before your period), progesterone levels rise significantly. Progesterone has a mild androgenic effect, meaning it can stimulate your sebaceous glands to produce more oil. At the same time, estrogen — which has a somewhat protective, anti-inflammatory effect on the skin — begins to drop. The result is a window of heightened oil production and increased inflammation, creating the perfect conditions for breakouts on oil-rich areas like the back.
This cyclical pattern is one of the hallmarks of hormonally driven acne and is a key reason why back acne in females often follows a predictable monthly rhythm.
PCOS and Androgen Excess
Polycystic ovary syndrome (PCOS) affects roughly 8-13% of women of reproductive age, according to the World Health Organization. One of its defining features is elevated androgen levels — particularly testosterone and its more potent derivative, dihydrotestosterone (DHT). These androgens directly stimulate the sebaceous glands to produce more sebum, which contributes to clogged pores and acne.
Back acne is particularly common in women with PCOS because the back and shoulders have a high density of androgen-sensitive oil glands. A study published in the Journal of Clinical and Aesthetic Dermatology found that acne in women with PCOS tends to be more resistant to standard treatments and is more likely to affect the trunk (back, chest, and shoulders) in addition to the face.
If your back acne is accompanied by other signs of androgen excess — such as irregular periods, thinning hair on the scalp, or excess hair growth on the face and body — it is worth discussing PCOS with your healthcare provider or dermatologist.
Stress and Cortisol
Chronic stress does not just feel terrible — it actively makes your skin worse. When you are stressed, your adrenal glands release cortisol, a hormone that triggers a cascade of skin-unfriendly effects. Cortisol stimulates sebaceous glands to produce more oil, promotes inflammation, and can even impair your skin's ability to heal. A study in Clinical, Cosmetic and Investigational Dermatology found a significant correlation between self-reported stress levels and acne severity in adult women.
While stress affects everyone, research suggests that women may be more susceptible to stress-related acne flares due to the interplay between cortisol and reproductive hormones. Cortisol can disrupt the balance of estrogen and progesterone, amplifying the hormonal fluctuations that already predispose women to breakouts.
Pregnancy and Postpartum Hormonal Shifts
Pregnancy brings dramatic hormonal changes that can trigger acne in women who have never dealt with it before — or worsen it in those who have. Rising progesterone levels during pregnancy, particularly in the first trimester, increase sebum production across the body. Some women find that their back acne improves in the second and third trimesters as estrogen levels rise, while others experience persistent breakouts throughout.
The postpartum period brings another hormonal upheaval. The sudden drop in estrogen and progesterone after delivery, combined with the stress and sleep deprivation of early parenthood, can trigger or worsen back acne for months.
Perimenopause and Menopause
Adult-onset acne, including back acne, is increasingly recognized as a common concern during perimenopause. As women approach menopause, estrogen levels decline while androgen levels remain relatively stable or decline more slowly. This shifting ratio means that androgens exert a proportionally stronger influence on the skin, driving increased oil production and breakouts — even in women who had clear skin throughout their 20s and 30s.
What to expect: Hormonal back acne in females tends to be deeper and more inflammatory than breakouts caused purely by external factors like friction or sweat. You are more likely to see painful nodules or cysts along the upper back and shoulders rather than surface-level whiteheads. If this sounds familiar, a dermatologist can help determine whether a hormonal treatment approach — like spironolactone — might be right for you.
Lifestyle and External Causes of Back Acne in Females
Hormones set the stage, but lifestyle factors often determine how severe your back acne actually gets. Many of these triggers are things you can control — once you know what to look for.
Tight Clothing and Sports Bras
Sports bras, activewear, and tight-fitting tops create friction and trap heat and sweat against the skin — a combination known as acne mechanica. For women who work out regularly, the band and straps of a sports bra sit directly over acne-prone areas of the upper back and shoulders, creating persistent pressure that can worsen breakouts. Synthetic fabrics that do not breathe compound the problem by holding moisture against the skin.
Hair Products Running Down the Back
Conditioners, hair oils, leave-in treatments, and styling products that rinse down your back in the shower can leave a pore-clogging residue on the skin. This is sometimes called "pomade acne," and it is a particularly common — and often overlooked — trigger for back acne in women with longer hair. The oils and silicones in these products can occlude pores and promote breakouts along the hairline and upper back.
Sweat and Delayed Showers
Sweat itself is not inherently acne-causing, but when it sits on the skin and mixes with oil, dead skin cells, and bacteria, it creates an environment that accelerates breakouts. Women who work out in the morning and then wait hours to shower, or who throw on regular clothes over a sweaty base layer, are particularly susceptible. The back, with its high oil gland density and limited air exposure under clothing, is ground zero for sweat-related flares.
Body Care Products
Heavy body lotions, sunscreens, and body oils can clog the pores on your back, especially if they contain comedogenic ingredients like coconut oil, cocoa butter, or certain silicones. Unlike facial skincare products, which are frequently formulated to be non-comedogenic, body products are not always designed with acne-prone skin in mind.
Diet and Inflammation
While diet alone does not cause acne, research suggests that certain dietary patterns may worsen hormonal acne in some women. A 2021 review in the Journal of the American Academy of Dermatology found associations between high-glycemic diets and increased acne severity. High-glycemic foods cause rapid spikes in blood sugar and insulin, which in turn can increase androgen activity and sebum production — adding fuel to the hormonal fire that drives back acne in females.
Red flag: If your back breakouts are uniform in size, intensely itchy rather than painful, and do not respond to typical acne treatments, you may be dealing with fungal folliculitis (sometimes called "fungal acne") rather than true acne. This condition is caused by yeast overgrowth, not bacteria, and requires a completely different treatment approach. A dermatologist can help you distinguish between the two.
Back Acne in Females vs. Males: Key Differences
Both males and females get back acne, but the causes, patterns, and timing tend to differ. Understanding these differences can help you seek the right treatment approach.
| Factor | Females | Males |
|---|---|---|
| Primary hormonal driver | Cyclical fluctuations in estrogen, progesterone, and androgens | Consistently higher baseline testosterone levels |
| Breakout pattern | Often cyclical, flaring before menstruation | Tends to be more persistent and constant |
| Peak age | Can persist or develop well into the 20s, 30s, and beyond | Often peaks during adolescence and improves in early 20s |
| Common associated conditions | PCOS, premenstrual syndrome, perimenopause | Anabolic steroid use, higher sebum production |
| Lifestyle triggers | Sports bras, hair products, hormonal skincare triggers | Heavy sweating, athletic gear, higher overall oil production |
| Adult acne prevalence | More common — adult acne affects women more than men | Less common after early adulthood |
One of the most important takeaways from this comparison is that back acne in females is more likely to be a long-term concern. Studies show that adult acne disproportionately affects women, with many experiencing breakouts into their 30s, 40s, and even 50s. If your back acne has persisted past your teenage years or started in adulthood, hormonal factors are very likely playing a significant role.
How to Treat Back Acne in Females
Effective treatment for back acne in females depends on what is driving it. For a detailed breakdown of all treatment options — including over-the-counter products, prescription medications, and lifestyle changes — see our complete guide on how to get rid of back acne. Below is a summary focused on approaches that are especially relevant for hormonally driven back acne in women.
Spironolactone for Hormonal Back Acne
If your back acne follows a hormonal pattern — flaring before your period, accompanied by jawline breakouts, or associated with PCOS — spironolactone is one of the most effective treatments available. Spironolactone works by blocking androgen receptors, reducing the hormonal signals that drive excess oil production. A systematic review in the Journal of the American Academy of Dermatology confirmed its effectiveness for adult acne in women, with most patients seeing improvement at doses of 50-100 mg daily.
For a deeper look at how spironolactone works for acne, including dosing, timeline, and what to expect, read our guide: Spironolactone for Acne: Everything You Need to Know.
Topical Retinoids and Benzoyl Peroxide
Topical treatments form the foundation of most acne regimens. Prescription retinoids like tretinoin accelerate cell turnover and prevent clogged pores, while benzoyl peroxide (available over the counter at 5-10% strengths) kills acne-causing bacteria. For back acne, a benzoyl peroxide body wash is one of the easiest and most practical first-line treatments since it covers a large area and rinses off in the shower.
Oral Antibiotics
For moderate inflammatory back acne, oral antibiotics like doxycycline can reduce bacteria and inflammation systemically. The American Academy of Dermatology recommends limiting antibiotic courses to 3-6 months to reduce the risk of resistance, and combining them with a topical like benzoyl peroxide.
Accutane (Isotretinoin)
For persistent back acne that has not responded to other treatments, Accutane (isotretinoin) is often the most effective option. Isotretinoin works by dramatically reducing sebum production, shrinking oil glands, and normalizing skin cell turnover — addressing every major factor behind acne. A typical course lasts 4-6 months, and a JAMA Dermatology study found that 97.4% of patients showed improvement at 12 months.
Lifestyle Adjustments
Regardless of which treatments you use, these habits can significantly reduce back acne flares:
Daily Habits to Reduce Back Acne
- Shower within 30 minutes of sweating — use a benzoyl peroxide or salicylic acid body wash
- Change out of sweaty sports bras and workout clothes immediately
- Clip hair up when conditioning, then wash your back last in the shower
- Choose non-comedogenic body lotions and sunscreens
- Wear loose, breathable fabrics — especially during exercise
- Wash sheets and pillowcases at least once per week
- Track breakout timing relative to your menstrual cycle to identify patterns
What to expect: If your back acne is hormonally driven, over-the-counter products alone are unlikely to fully clear it. They can reduce the severity and manage surface-level breakouts, but addressing the hormonal root cause typically requires prescription treatment. Most women with hormonal back acne see the best results with a combination approach — for example, spironolactone to address the hormonal component plus a topical retinoid or benzoyl peroxide for maintenance.
When to See a Dermatologist for Back Acne
While mild, occasional back breakouts can often be managed with OTC products and lifestyle changes, certain patterns warrant professional evaluation:
- Your back acne flares consistently before your period or follows a hormonal pattern
- You have deep, painful cysts or nodules on your back
- Over-the-counter treatments have not improved your breakouts after 2-3 months
- Your back acne is leaving dark marks or scars
- You suspect PCOS or another hormonal condition may be contributing
- Back acne developed or significantly worsened in adulthood
At Honeydew, our board-certified dermatologists, nurse practitioners, and physician assistants have treated over 100,000 acne cases, including many women dealing with hormonally driven back acne. We can evaluate your breakout patterns, determine whether hormonal factors are playing a role, and build a personalized treatment plan that might include spironolactone, prescription topicals, oral medications, or isotretinoin — depending on your specific situation.
We offer same-day and next-day video appointments, so you do not have to wait weeks for an in-person visit. Our membership starts at $39/month, and you can message your care team anytime with questions about your treatment.